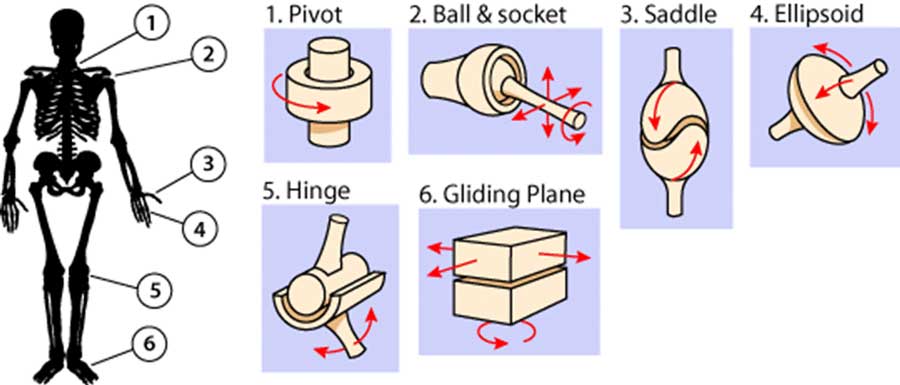
A Joint Venture Into Staying Mobile
Since I’m doing the writing and you’re doing the reading, we’re in this together. So. Let’s jointly venture forth and learn about how to keep our joints healthy. I don’t want to saddle you with too much information. Much of what it takes to keep gliding smoothly through the physical plane of our existence hinges on controlling inflammation. I might need to pivot sharply to cover everything I want to cover and I might omit some things, hopefully without being too elliptical. (Sadly, I wasn’t hip enough to figure out a way to work in “ball and socket”).
Osteoarthritis (OA) is the most common joint problem facing us as we age, and this post will focus on it. Other joint problems arise from acute or repetitive trauma, inflammation due to infection or autoimmune disease, compromise of the blood supply to the bones, medication side effects and other more esoteric causes but ultimately there is always inflammation and damage.
Here’s a very simplistic diagram of a joint connecting unidentified long bones, just to get us moving:
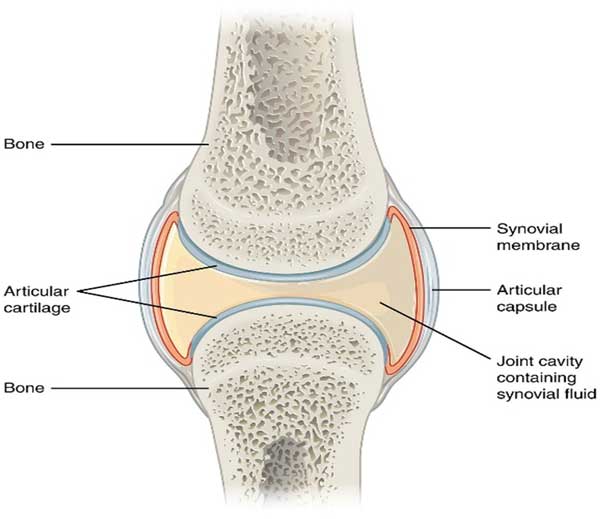
The joint is enclosed in a membranous capsule or synovium containing goopy, viscous fluid resembling egg whites. This synovial fluid provides nutrients, receives signals from elsewhere in the body, and acts as a lubricant and shock absorber. It’s a filtrate of blood plasma, courtesy of the synovial membrane.
The articulating surfaces of the bones are sheathed in cartilage: a spongy four-layered living tissue which is like Teflon. Cartilage has no blood supply and nutrients diffuse into it from the synovial fluid. Cartilage consists of cells called chondrocytes surrounded by a matrix of various proteins secreted by the chondrocytes. The surrounding matrix is referred to as the ECM or Extracellular Matrix. It’s important to point out that the chondrocytes don’t regenerate well over time (Note that if we were referring to the iconic Keanu Reeves Hollywood film tetralogy, ECM would stand for Extremely Confusing Movies).
This diagram illustrates the composition of the ECM:

It’s a bit of a jungle in there, with collagen protein strands crisscrossed with hyaluronic acid strands. The hyaluronic acids are long chains of repeating units of sugars strung together like pearls in a necklace. One of the repeating sugars is a modified form of glucosamine, often included in joint supplement formulas.
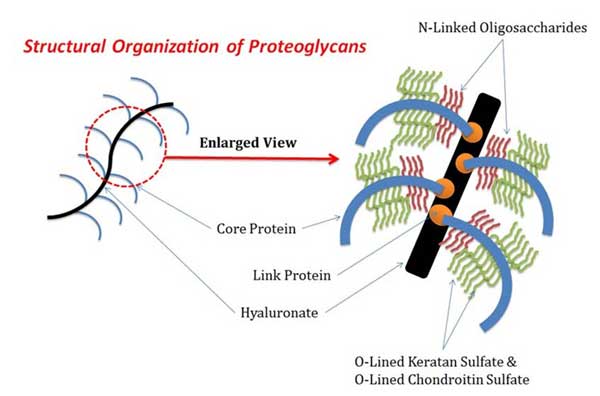
The furry, caterpillar-like things attached to the hyaluronic acid strands are proteoglycans. Proteoglycans are the molecular love children of other proteins (chondroitin, keratan) and very short chains of sugars known as oligosaccharides. All these structures can electrically attract and hold water molecules helping to maintain the sponginess and resiliency of the cartilage.
So, what was the point of my explaining all this to you? My point is that all these ECM chains and complex structures of various description routinely break down and need to be replaced. The chondrocytes “renovate” the ECM until they start to fail. Then the trouble begins.
There is a genetic aspect to OA, not completely sussed out, leading to a greater tendency for some people to develop OA but we all accumulate some osteoarthritic changes in our joints over time. OA was thought to arise simply due to “wear and tear” but it’s more complicated than that. In OA, cartilage begins to deteriorate and dry out: chondrocytes lose their function: the bone underlying the cartilage becomes fibrotic and grows irregular bony outcroppings called osteophytes. The changes described are accompanied by inflammation mediated by the chondrocytes and immune cells in the synovial membrane. Therefore, approaches to prevention and mitigation of OA damage revolve around suppression of inflammation and provision of nutrients that can support the chondrocytes and the ECM. For example, a blend of chondroitin sulfate and glucosamine, targeting the ECM, is in wide use for OA.
I want to reiterate one thing before moving on to talk about interventions. When we last spoke, I pointed out that to protect bone from fractures you need adequate muscle bulk and strength but really, muscle helps protect the integrity of the entire unit: bones, joint cartilage and joint capsule in the face of sudden impacts and the stresses imposed by exercise and other routine activities such as gymnastic tumbling. Muscle is actually an endocrine organ secreting signaling molecules that regulate the function of other organs and the immune system. Generally, if you’re not able to maintain muscle for whatever reason, you’re going to have joint problems eventually.
Treatment of OA
I won’t spend much time on the pharmaceutical approaches to joint inflammation which we’re all familiar with. The mainstay non-steroidal anti-inflammatory drugs, or NSAIDs, interfere with formation of prostaglandins, molecules that play a role in inflammation. NSAIDs are famous for gastrointestinal side effects, other side effects and over the long haul, depletion of nutrients such as copper, which is important for collagen elasticity. Another tactic used is a periodic injection of hyaluronic acid into afflicted joints (used primarily for knees). Neither of these approaches does anything to actually support the afflicted joints.
We have accumulated a large body of anecdotal evidence involving herbs and herbal extracts which appear to do the same thing as the NSAIDs, without the harm. For the most part, all these time-tested remedies block steps in the cascade of events that lead to inflammation and/or scavenge destructive free radicals that arise with inflammation. Some remedies contain nutrients needed to support the joint tissues. These products are still around after traditional usage spanning thousands of years in some cases.
What about scientific evidence for traditional remedies? Liu et al performed a meta-analysis, examining approximately 3000 papers and summarizing the results from the 69 highest-quality studies (Liu 2017). The drawbacks to the natural product studies that have been done is that most studies last only a few months and don’t have thousands of participants. Funding of studies on products that are not patentable is hard to come by. The other problem with the Liu study is that it only settled on products with a single ingredient. More on that in a minute.
A paper by Colletti et al discusses the literature on mechanisms of action for a variety of supplements (Colletti 2021). You have my blessing to read that paper if you’re into mechanisms. A review article by Hector Lopez MD is an excellent discussion of essential fatty acids for OA with emphasis on fish oil (Lopez HL. Part I) whereas a companion article discusses micronutrients and other supplements (Lopez HL. Part II). Micronutrients include boron, selenium, copper, zinc and manganese. Other supplements include Vitamin C, Vitamin K2, Vitamin D, N-acetylcysteine, and proteolytic enzymes.
Joint formulas typically contain a blend of many ingredients, and these may often work better than single ingredient formulations due to the synergistic effect of multiple mechanisms. The amounts of any one ingredient in a blend tend to be lower and this minimizes the chance of adverse effects.
Your Integrative/Restorative Medical practitioner can advise you about what supplements have worked the best in their practices. There is no one best approach. Treating inflammation is like making soup: adding some of this, some of that and some of the other makes for the best taste.
I’m going to recommend three foundational “soup” ingredients based on my own experience. Then I’ll shut up!
Methylsulfonylmethane (MSM), SeaCuMax, Niacinamide
Long story short: I’ve been on a fairly stiff dose of methylsulfonylmethane (MSM) for more than 20 years accompanied by a whole-food product called SeaCuMAX. Despite pounding the heck out of my knees and hips for more than fifty years, I have no persistent arthritic symptoms in those joints. I’ve recommended combinations of the above two supplements to many patients and friends over the years, to good effect. I added Niacinamide to the list in early 2022.
I held forth on MSM in a previous post so no need to repeat that detail here. Many of the patients I gave it to reported ongoing improvement in joint pain and swelling from OA with no or transient side effects. While I take 2000 mg twice daily, none of the studies I’ve seen go above 1000-2000 mg/day. There are studies indicating that MSM intervenes in the same inflammatory signaling pathways as do powerful prescription steroids such as prednisone and dexamethasone (Ahn 2015). Although the received wisdom is that chondrocytes don’t regenerate, a 2021 study by Dalle Carbonare et al (human stem cells and zebrafish) indicates that MSM might play a role in promoting formation of new chondrocytes from stem cell progenitors (Dalle Carbonare 2021). MSM also fared well in the meta-analysis (Liu) I mentioned, with three high quality randomized, controlled trials indicating improved pain relief and functioning.
SeaCuMAX is a product developed by Pete Collin, a self-taught marine biochemist and sustainable farmer of cold-water sea cucumbers. It’s available from his company, Coastside Bio Resources: https://coastsidebio.com/seacumax/. SeaCuMAX is made from the dried and powdered flesh of the Cucumaria frondosa species, pictured below. Although warm-water sea cucumbers have been eaten for thousands of years, it is the cold-water animals which pack an anti-inflammatory punch.

Along with being a whole food rich in trace elements, sea cucumbers have many interesting constituents including some interesting marine lipids and fucosylated chondroitin sulfate (FCS), a unique form of chondroitin sulfate found only in sea cucumbers. Pomin et al discuss the anti-inflammatory properties (and many other properties) of FCS (Pomin 2014).
I learned about Pete through a patient of mine and eventually met him in the late 1990’s. Since then, I have dispensed boatloads of SeaCuMAX to patients with OA, Rheumatoid Arthritis, Lupus Arthritis, Psoriatic Arthritis and Ankylosing Spondylitis. SeaCuMAX takes a month or two to kick in but has improved the lives of many people I know. The dose is 3 capsules twice a day. I have always taken it with food since it is a food.

Pete Collin (left) and the author, many years ago!
Last but not least: Nicotinamide aka Niacinamide. I sprained my left thumb cross-country skiing when I was in my 20’s. Despite all the MSM and SeaCuMAX, I developed pain and clicking in the carpometacarpal joint at the base of that thumb a few years ago. For some reason, that joint is apparently the most common site for OA. No one knows why. Anyway, the discomfort cleared up several months after I started Nicotinamide 500 mg twice daily, in early 2022. At this point, any minimally-skeptical person would say, “So what? That’s an anecdote.”
True, but alert readers will recall that I talked about nicotinamide in the context of skin health, and anti-aging last month. I also mentioned the work of William Kaufman, MD, PhD. For ten years spanning WWII, the good doctor gave nicotinamide to over 650 of his patients in divided doses ranging from 1 to 4 grams daily. He saw clear improvements in grip strength, endurance and the aggregate range of motion based on precise measurements at the neck, shoulders, wrists, fingers, hips and knees. The therapy was shown to be safe and effective (Kaufman 1955).
In 1996, other researchers, citing Kaufman’s work, also studied nicotinamide specifically for OA at a total daily dose of 3000 mg and saw increases in joint mobility, decreased ESR (a marker of inflammation) and decreased overall impact of OA (pain and quality of life) with minimal GI side effects (Jonas 1996). All in all, I’m not surprised that the nicotinamide did have a beneficial effect on my left thumb!
Closing comments
I think I’ve given a good overview of joint health despite limited space but I want to give a quick nod to more recent therapies. These include peptides (small protein chains) and autologous stem cell injections that can trigger chondrocyte regrowth/cartilage repair. There are various devices generating red laser light at precise frequencies that can help trigger healing.
I didn’t expect that readers would come away from this post completely equipped to manage their joint problems on their own. But I think you now know enough to work with your Integrative/Restorative Medicine Practitioner to improve and maintain your joint health for many years to come.

Author: George Gillson, MD, PHD, CCFP
EvolveWell Medical Director
References
Ahn H, Kim J, Lee MJ, Kim YJ et al. Methylsulfonylmethane inhibits NLRP3 inflammasome activation. Cytokine. 2015 Feb;71(2):223-31. doi: 10.1016/j.cyto.2014.11.001. Epub 2014 Nov 21. PMID: 25461402.
Akkiraju H, Nohe A. Role of Chondrocytes in Cartilage Formation, Progression of Osteoarthritis and Cartilage Regeneration. J Dev Biol. 2015 Dec;3(4):177-192. doi: 10.3390/jdb3040177. Epub 2015 Dec 18. PMID: 27347486; PMCID: PMC4916494.
Colletti A, Cicero AFG. Nutraceutical Approach to Chronic Osteoarthritis: From Molecular Research to Clinical Evidence. Int J Mol Sci. 2021 Nov 29;22(23):12920. doi: 10.3390/ijms222312920. PMID: 34884724; PMCID: PMC8658017.
Dalle Carbonare L, Bertacco J, Marchetto G et al. Methylsulfonylmethane enhances MSC chondrogenic commitment and promotes pre-osteoblasts formation. Stem Cell Res Ther. 2021 Jun 5;12(1):326. doi: 10.1186/s13287-021-02396-5. PMID: 34090529; PMCID: PMC8180127.
Debbi EM, Agar G, Fichman G et al. Efficacy of methylsulfonylmethane supplementation on osteoarthritis of the knee: a randomized controlled study. BMC Complement Altern Med. 2011 Jun 27;11:50. doi: 10.1186/1472-6882-11-50. PMID: 21708034; PMCID: PMC3141601.
Ezaki J, Hashimoto M, Hosokawa Y et al. Assessment of safety and efficacy of methylsulfonylmethane on bone and knee joints in osteoarthritis animal model. J Bone Miner Metab. 2013 Jan;31(1):16-25. doi: 10.1007/s00774-012-0378-9. Epub 2012 Aug 10. PMID: 23011466.
Jonas WB, Rapoza CP, Blair WF. The effect of niacinamide on osteoarthritis: a pilot study. Inflamm Res. 1996 Jul;45(7):330-4. doi: 10.1007/BF02252945. PMID: 8841834.
Kaufman W. The use of vitamin therapy to reverse certain concomitants of aging. J Am Geriatr Soc. 1955 Nov;3(11):927-36. doi: 10.1111/j.1532-5415.1955.tb00947.x. PMID: 13271047.
Kim LS, Axelrod LJ, Howard P et al, Efficacy of methylsulfonylmethane (MSM) in osteoarthritis pain of the knee: a pilot clinical trial. Osteoarthritis Cartilage. 2006 Mar;14(3):286-94. doi: 10.1016/j.joca.2005.10.003. Epub 2005 Nov 23. PMID: 16309928.
Kloesch B, Liszt M, Broell J et al. Dimethyl sulphoxide and dimethyl sulphone are potent inhibitors of IL-6 and IL-8 expression in the human chondrocyte cell line C-28/I2. Life Sci. 2011 Sep 26;89(13-14):473-8. doi: 10.1016/j.lfs.2011.07.015. Epub 2011 Jul 28. PMID: 21821055.
Liu X, Machado GC, Eyles JP et al. Dietary supplements for treating osteoarthritis: a systematic review and meta-analysis. Br J Sports Med. 2018 Feb;52(3):167-175. doi: 10.1136/bjsports-2016-097333. Epub 2017 Oct 10. PMID: 29018060.
Lopez HL. Part I. Nutritional interventions to prevent and treat osteoarthritis. Part I: focus on fatty acids and macronutrients. PM R. 2012 May;4(5 Suppl):S145-54. doi: 10.1016/j.pmrj.2012.02.022. PMID: 22632694.
Lopez HL. Part II. Nutritional interventions to prevent and treat osteoarthritis. Part II: focus on micronutrients and supportive nutraceuticals. PM R. 2012 May;4(5 Suppl):S155-68. doi: 10.1016/j.pmrj.2012.02.023. PMID: 22632695.
Lubis AMT, Siagian C, Wonggokusuma E et al. Comparison of Glucosamine-Chondroitin Sulfate with and without Methylsulfonylmethane in Grade I-II Knee Osteoarthritis: A Double Blind Randomized Controlled Trial. Acta Med Indones. 2017 Apr;49(2):105-111. PMID: 28790224.
Pomin VH. Holothurian fucosylated chondroitin sulfate. Mar Drugs. 2014 Jan 9;12(1):232-54. doi: 10.3390/md12010232. PMID: 24413804; PMCID: PMC3917272.
Żęgota Z, Goździk J, Głogowska-Szeląg J. EFFICACY OF HERBAL AND NATURALLY-DERIVED DIETARY SUPPLEMENTS FOR THE MANAGEMENT OF KNEE OSTEOARTHRITIS: A MINI-REVIEW. Wiad Lek. 2021;74(8):1975-1983. PMID: 34537753.
