
Some Things to Think About As We Enter Cold/Flu Season
In the last post, I threatened to talk more about Immunity, so here goes.
I really didn’t know what to say, as Immunity is such a broad topic but since hormone balancing and hormone replacement are one of the main areas of focus at EvolveWell, I decided to delve into the role of steroid hormones in Immunity. Now I wish I hadn’t as the subject matter got pretty murky.
Benjamin Franklin once said: “Don’t put off until tomorrow what you can do today.” In my case, it’s more like: “Never do today what you can put off until tomorrow, especially when you are dealing with murky subject matter.”
The truth is that steroid hormone receptors (sex hormone and cortisol receptors) are littered all over the landscape of the immune system like the aftermath of a bad skiing wipeout. In other words, ALL the cells related to the immune system bear these receptors. There are interlocking and complementary feedback pathways everywhere and it’s impossible to determine causality/identify prime movers.
We know that there are sex differences in how the immune system operates, witnessed by the increased tendency toward autoimmunity in biological females (Moulton 2018). For example, the incidence of autoimmune conditions including Multiple Sclerosis, thyroiditis, Sjogren’s Syndrome and Rheumatoid Arthritis is significantly higher in females relative to males and this is in part influenced by estrogens. However, during pregnancy, women are somewhat immunosuppressed (to avoid rejection of the fetus) and may experience remission of some autoimmune conditions. Paradoxically, lupus, another autoimmune condition, may worsen during pregnancy.
Long story short, autoimmunity is heavily influenced by sex hormones and although that’s interesting, it’s not all that relevant here at the beginning of Viral Respiratory Infection Season aka Fall.
So.
What do we know about viral infections and steroid hormones? Well, we know that there are correlations to sex and sex hormone levels for at least one viral infection: SARS-CoV-2.
Per Su et al (Su 2022):
Anyway, there are numerous other lessons to be learned here. Well, maybe not numerous lessons, but a couple for sure.
The first lesson is that if there’s someone you have known for more than forty years, and whom you have trusted as a wise Family Doctor for twenty-five years, you should probably do what they tell you to do straight away, instead of waiting for several months.
“Sex differences in COVID-19 vulnerability and clinical manifestations have been observed by various studies. It has been well established that SARS-CoV-2-infected males have significantly higher rates of progressing into severe diseases, and male-to-female fatality ratios obtained from different countries are between 1.7-1.8. “
We know that in males, viral infection with increased release of cytokines (immune response-influencing molecules) such as IL-1, IL-6 and TNF-alpha will suppress testosterone production. That’s not good, as testosterone is somewhat anti-inflammatory. There is some evidence that supplementation with testosterone in the face of SARS-CoV-2 infection can mitigate the illness, especially in older males (Auerbach 2021, Mohamad 2019).
This diagram from Mohamad et al depicts the complex role that testosterone plays in immune response:
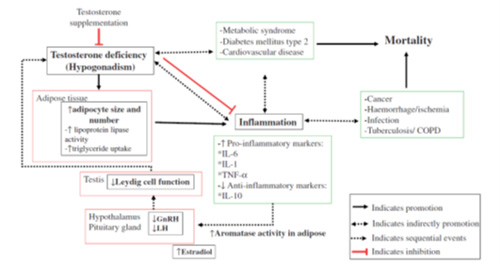
There won’t be a test on that diagram.
: )
We’re just not sure whether low testosterone increases your risk of becoming infected, or whether an infection lowers testosterone due to the resulting inflammation. Further studies are needed to delineate the role of testosterone supplementation before and during acute viral respiratory infections.
Whereas testosterone may drop during certain viral infections, progesterone increases, at least in animal studies, with exposure to various respiratory viruses (Su 2022).
“Our discovery that progesterone is induced following viral infection and promotes innate antiviral responses provides an explanation for the observations that SARS-CoV-2-infected females have reduced severity and fatality in comparison to males. Our study indicates that the progesterone levels are negatively correlated with the severity of COVID-19. It is possible that heightened innate immune response in SARS-CoV-2-infected patients accompanied by higher levels of progesterone contributes to the alleviated symptoms of COVID-19.“
The authors go on to say that progesterone may have dose-dependent effects, promoting a stronger immune response at one level and restraining inflammatory responses at a higher level. Achieving a more youthful but not excessive increase in progesterone might be an effective strategy.
From a personal perspective, I can also talk about the role of cortisol in immunity. As we all know, cortisol is anti-inflammatory. Unrestrained inflammation, whether from overtraining, gut inflammation/leaky gut or perhaps a toxin exposure will cause the immune system to “pay too much attention” and perhaps lead to an autoimmune condition if left untreated. In my case, my cortisol production over the last couple of years has been quite low, as witnessed by low cortisol and cortisone metabolites on 24-hour urine steroid testing. This may have contributed to my development of Polymyalgia Rheumatica as discussed in previous posts.
This was a hard post to write. Steroid hormones are intimately involved in the functioning of the immune system but it’s very complex. The best I can say is that if you are concerned about the functioning of your immune system with regard to autoimmunity or if you are concerned about “Flu Season”, a great way to begin would be to visit your EvolveWell Integrative/Functional Medicine practitioner and optimize your steroid hormone status with the aid of a comprehensive 24-hour urine steroid hormone assay.
P.S. In a previous post, I said this:
“I’m thinking about adding some pregnenolone at bedtime. Pregnenolone is much easier on the body than prednisone as it can convert into cortisol, progesterone, DHEA and testosterone, providing anti-inflammatory and anabolic effects at the same time. It was used more than 60 years ago to treat rheumatoid arthritis but I’ll be darned if I can find that paper. “
Well, I found a trove of papers, circa 1950, on the topic and the references are listed at the bottom of the list of other papers I cited in this post. I would be happy to provide PDFs of those papers upon request.

Author: George Gillson, MD, PHD, CCFP
EvolveWell Medical Director
General References
Auerbach JM, Khera M. Testosterone’s Role in COVID-19. J Sex Med. 2021 May;18(5):843-848. doi: 10.1016/j.jsxm.2021.03.004. Epub 2021 Mar 19. PMID: 33903045; PMCID: PMC7972673.
Mohamad NV, Wong SK, Wan Hasan WN et al. The relationship between circulating testosterone and inflammatory cytokines in men. Aging Male. 2019 Jun;22(2):129-140. doi: 10.1080/13685538.2018.1482487. Epub 2018 Jun 21. PMID: 29925283.
Moulton VR. Sex Hormones in Acquired Immunity and Autoimmune Disease. Front Immunol. 2018 Oct 4;9:2279. doi: 10.3389/fimmu.2018.02279. PMID: 30337927; PMCID: PMC6180207.
Su S, Hua D, Li JP et al. Modulation of innate immune response to viruses including SARS-CoV-2 by progesterone. Signal Transduct Target Ther. 2022 Apr 25;7(1):137. doi: 10.1038/s41392-022-00981-5. PMID: 35468896; PMCID: PMC9035769.
Yassin A, Sabsigh R, Al-Zoubi RM et al. Testosterone and Covid-19: An update. Rev Med Virol. 2023 Jan;33(1):e2395. doi: 10.1002/rmv.2395. Epub 2022 Sep 3. PMID: 36056748; PMCID: PMC9537909.
References pertaining to the treatment of Rheumatoid Arthritis with pregnenolone
Fisk GH, Howard RP, ay K. Rheumatoid arthritis. I. Clinical effects of testosterone and pregnenolone therapy. Can Med Assoc J. 1950 Oct;63(4):342-4. PMID: 14778063; PMCID: PMC1821768.
Freeman H, Pincus G, Bachrach S, Johnson CW, McCabe GE, MacGilpin HH Jr. Oral steroid medication in rheumatoid arthritis. J Clin Endocrinol Metab. 1950 Dec;10(12):1523-32. doi: 10.1210/jcem-10-12-1523. PMID: 14803541.
Howard RP, Venning EH, Fisk GH. Rheumatoid arthritis. II. Studies of adrenocortical and hypophyseal function and the effects thereon of testosterone and pregnenolone therapy. Can Med Assoc J. 1950 Oct;63(4):340-2. PMID: 14778062; PMCID: PMC1821761.
Myers GN. Pregnenolone in the treatment of rheumatoid arthritis. Ann Rheum Dis. 1951 Mar;10(1):32-45. doi: 10.1136/ard.10.1.32. PMID: 14819947; PMCID: PMC1030626.
Trumble BC, Blackwell AD, Stieglitz J et al. Associations between male testosterone and immune function in a pathogenically stressed forager-horticultural population. Am J Phys Anthropol. 2016 Nov;161(3):494-505. doi: 10.1002/ajpa.23054. Epub 2016 Jul 28. PMID: 27465811; PMCID: PMC5075254.
