
Stress Reduction (Part 2): How To Manage What You Measure
In the previous post, I introduced Precision Analytical Laboratory’s DUTCH urine steroid hormone assay, an innovative test which can assess the hour-by-hour variation of free cortisol and at the same time gauge the total output across a 24-hour cycle for all steroid hormones including cortisol. This approach, although originated by Precision Analytical, is now being adopted by most of the other laboratories doing urine hormone testing, due to its versatility.
For those of you who didn’t read that post, I used the following metaphors:
”Cortisol is produced in pulses throughout the day. It’s distributed to tissues, delivers its messages and is then rapidly broken down by the liver into inactive cortisol metabolites and excreted mostly in urine. This seems wasteful but it enables the adrenal glands to rapidly adjust cortisol output to changing demand. Measurement of the cortisol metabolites has been shown to reflect production of cortisol. A good analogy would be to look in someone’s blue bin to determine how much stuff they order from Amazon by counting wrappers and cardboard boxes.
The other cortisol measurement that is important in urine is free cortisol, which is thought to reflect what the bodily tissues are exposed to at any given time. It’s the difference between peering into the blue bin every few hours versus peering into it every other day or so. Another analogy might be that the cortisol metabolites are your salary and free cortisol is what’s in your wallet or purse at any given time.”
Recall that I also exercised artistic license by taking the Morning point (A) point from the standard 4-point free cortisol graph and “replaying” it at the right end of the graph as (A*), to help you picture what is going on with your free cortisol while you’re sleeping. (Remember that you can’t feasibly get this information from saliva or serum testing!) Once again, on the actual reports you only see the A,B,C and D points.
Without further ado, let’s take a look at the profiles I introduced last time in more detail.

The “Bottom Feeder” profile indicates that there is very little free cortisol being produced as the green patient line hugs the bottom end of the normal ranges. The profile does display an increase in cortisol overnight and a modest surge in cortisol after waking (A to B). The missing piece here is how much cortisol the patient makes over 24 hours. This person may be a short/petite/slender individual who simply makes less cortisol overall because they have a small body that doesn’t need as much cortisol as the average person. They may feel just fine.
However, complaints of fatigue, brain fog, poor tolerance for physical exertion, waking up unrefreshed, dizziness upon standing, fearful anxiety (“I am on my last nerve and If one more thing happens, I am going to snap”) with a “bottom feeder” profile indicate a need for further testing. There might be a problem with the adrenal glands, altered signaling between the brain and the adrenal glands, burnout from weight loss/calorie restriction and/or over-exercising and/or nutrient depletion. There might also be an issue with the liver such as cirrhosis or inflammation. If the liver can’t properly break down cortisol this can culminate in reduced cortisol production by the adrenals.
Long story short, a thorough history needs to be taken and additional testing might be warranted. Faced with a situation like this, your Integrative Health practitioner wouldn’t simply prescribe supplementation with cortisol. Some patients like this simply need to gear down and rest, if no other cause can be found. Energizing adrenal supplements as well as pantothenic acid, vitamin C and trace elements may help restore cortisol production.

The “Redliner” profile reveals that this individual is producing a large amount of free cortisol since all the (green) points lie above the high end of the normal range (red line). There is also very large increase in free cortisol overnight accompanied by only a small additional increase after waking. (Normally the result for the B point is 1.5 to 3 times the result for the A point.)
If this type of profile is accompanied by 24-hour cortisol production that is also well above the high end of the normal range, your practitioner needs to rule out Cushing’s Syndrome aka Hypercortisolism, with further testing. This situation can be accompanied by an increase in body fat, an accumulation of fat at the back of the neck, high blood pressure, bone loss and problems regulating insulin and blood sugar. Treatment depends on the cause such as a pituitary tumor or adrenal tumor.
If this is not the case, this profile might be seen in someone who is inherently Type A, driven, always “on”, or someone who is in a high-stress job, in a caregiver role, going through a divorce or financial problems. Patients like this may have insulin-glucose regulation issues (Metabolic Syndrome, Insulin Resistance). This profile occasionally be seen with stimulant medication or uncontrolled chronic pain. Lifestyle changes to reduce or eliminate stress might be in order.
There are a variety of calming supplement formulations such as Sereni-Pro that might be recommended by your Integrative Medicine practitioner. Melatonin supplementation helps to lower cortisol at night. A supplement called phosphatidyl serine also helps the brain to become more sensitive to cortisol and better able to regulate cortisol production.
Left alone, this “overdrive” situation could eventually lead to health problems such as diabetes, high blood pressure, obesity and cognitive decline.

In a “Sprinter” profile, all the cortisol production is concentrated in the period from waking to bedtime. Little cortisol is made overnight, resulting in poor sleep. Just the same, the patient may literally leap out of bed, “sprint” through the day and collapse into bed that night, out of “gas”. This person could have started out with a “Redlner” profile and is now on their way to developing a “Bottom Feeder” profile.
A good history around sleep hygiene/sleep quality would be needed to troubleshoot this. Calming supplements such as Sereni-Pro and Cortisol Manager early in the day might be in order whereas an energizing supplement (e.g. Rhoziva, Adapten-All, Adreset) might be used later in the day. Low-dose licorice extract at bedtime may increase cortisol. (Some energizing supplements listed may already contain licorice.)
It may be helpful in some instances to prescribe a small amount of cortisol at bedtime (<5 mg). Patients suffering from Addison’s Disease, an inability to make cortisol, take supplemental prescription cortisol to replace what they can’t make. It’s been shown that these patients have better quality sleep when given a small dose at bedtime (García-Borreguero 2000).
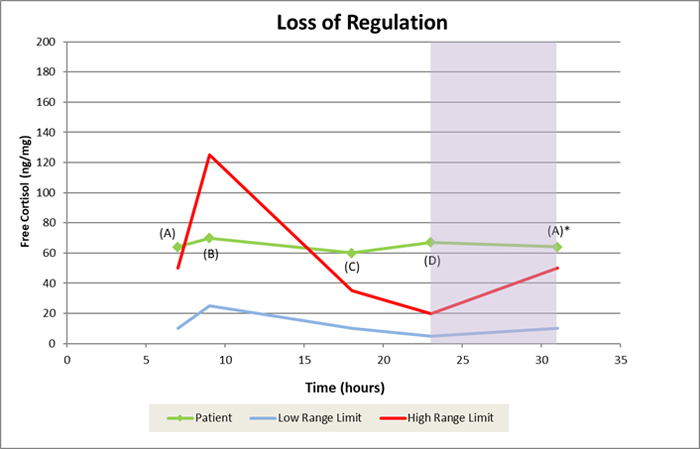
The “Loss of Regulation” profile indicates just that: little or no variation across 24-hours. One of the common causes of this is shiftwork, swing shifts in particular. Given time, the brain and body can adapt to habitual evening or night shifts but continually changing from day shifts to evenings to night shifts eventually disrupts the normal “clock”. Pilots and flight attendants can also exhibit a loss of regulation for the same reason.
This is a list of causes taken from Potter et al 2016:
- Work schedule (e.g. shift work, social jetlag, early school start times)
- Jetlag
- Unusual photoperiods (e.g. Polar regions)
- Circadian rhythm sleep-wake disorders (e.g. noon-24-hour sleep-wake disorder)
- Senescene
- Disease states (e.g. Alzheimers, Smith-Magenis syndrome
Mood disorders including major depressive disorders, anxiety disorders and bipolar disorder may also cause loss of cortisol regulation (Potter 2016).
Dysregulated cortisol patterns left untreated increase the risk of insulin resistance, Type II diabetes and overall increased inflammation and reduced immune function. These are recipes for heart disease and cancer.
Treatment involves identifying the primary cause, making appropriate lifestyle modifications, as well as instituting light therapy and melatonin if indicated.
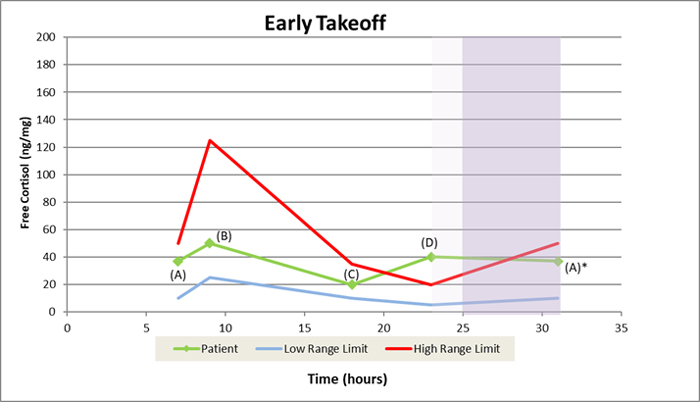
I refer to this last pattern as “Early Takeoff” because free cortisol drops from the morning peak until suppertime (B to C) but then rises until bedtime (C to D) and continues rising throughout the night. It’s like a plane landing, taxiing and then taking off again too soon. This pattern may reflect the “second shift” phenomenon: the stress that arises when people come home from work and are then occupied with all the other tasks such as meal preparation, children’s extracurricular activities, household chores and so forth.
It may also reflect an issue with light exposure. Normally, as daylight fades, melatonin begins to rise (this is known as Dim Light Melatonin Onset or DLMO) and this helps to suppress cortisol until several hours into sleep. Too much bright light exposure/too much screen-time/falling asleep in front of a laptop in the latter part of the evening can result in failure to suppress cortisol. Reducing your evening light “dosage” and/or supplementation with melatonin can help keep a lid on cortisol until the appropriate time for it to rise.
Conversely, and this wasn’t addressed earlier, people who can’t seem to get started in the morning may benefit from bright light exposure upon awakening with the aid of one of the various light therapy visors, glasses and lamps used to treat Seasonal Affective Disorder. This suppresses lingering melatonin and helps to amplify the Awakening Response discussed earlier.
Well, this brings the discussion of cortisol profiling via urine testing to a close but only scratches the surface of the many ways in which urine steroid hormone testing is useful. I’ve mentioned that all urine steroid testing labs are also able to quantify the total amounts of many different hormones produced over a 24-hour cycle. Urine measurement of the other steroid hormones such as testosterone, estradiol, progesterone and DHEA can also help you and your Integrative Medicine practitioner to better understand and rectify stress-related health issues.
Look for more discussion of the role of urine steroid hormone testing in the New Year.
All the best in 2023!

Author: George Gillson, MD, PHD, CCFP
EvolveWell Medical Director
References
García-Borreguero D, Wehr TA, Larrosa O et al. Glucocorticoid replacement is permissive for rapid eye movement sleep and sleep consolidation in patients with adrenal insufficiency. J Clin Endocrinol Metab. 2000 Nov;85(11):4201-6. doi: 10.1210/jcem.85.11.6965. PMID: 11095454.
Potter GD, Skene DJ, Arendt J et al. Circadian Rhythm and Sleep Disruption: Causes, Metabolic Consequences, and Countermeasures. Endocr Rev. 2016 Dec;37(6):584-608. doi: 10.1210/er.2016-1083. Epub 2016 Oct 20. PMID: 27763782; PMCID: PMC5142605.
Walker WH 2nd, Walton JC, DeVries AC, Nelson RJ. Circadian rhythm disruption and mental health. Transl Psychiatry. 2020 Jan 23;10(1):28. doi: 10.1038/s41398-020-0694-0. PMID: 32066704; PMCID: PMC7026420.
